
Medical Device
Medical Device Coordination Group Document MDCG 2024-3
1
MDCG 2024-3
Guidance on content of the Clinical
Investigation Plan for clinical
investigations of medical devices
March 2024
This document has been endorsed by the Medical Device Coordination Group (MDCG)
established by Article 103 of Regulation (EU) 2017/745. The MDCG is composed of
representatives of all Member States and it is chaired by a representative of the
European Commission. The document is not a European Commission document and it
cannot be regarded as reflecting the official position of the European Commission. Any
views expressed in this document are not legally binding and only the Court of Justice
of the European Union can give binding interpretations of Union law.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
2

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
3
Table of contents
Abbreviations ..................................................................................................................................................... 4
1. Introduction................................................................................................................................................. 5
2. Purpose of the CIP .................................................................................................................................... 6
3. Content of the CIP ..................................................................................................................................... 6
3.1. General ................................................................................................................................................ 6
3.2. Identification and description of the investigational device .......................................................... 7
3.3. Benefits and risks of the investigational device, clinical procedures and clinical investigation .. 8
3.3.1. Benefits ................................................................................................................................................ 8
3.3.2. Risks ..................................................................................................................................................... 9
3.3.3. Benefit-risk ratio ................................................................................................................................ 10
3.4. Relevance of the clinical investigation ........................................................................................... 10
3.5. Objectives and hypotheses ............................................................................................................. 11
3.6. Design of the clinical investigation ................................................................................................. 11
3.6.1. General information such as type of investigation with rationale for choosing it, for its
endpoints and for its variables as set out in the clinical evaluation plan ................................................... 11
3.6.2. Information on the investigational device and any comparator to be used in the clinical
investigation. ...................................................................................................................................................... 12
3.6.3. Information on subjects, selection criteria, size of investigation population, representativeness
of investigation population in relation to target population and, if applicable, information on vulnerable
subjects involved such as children, pregnant women, immuno-compromised or elderly subjects. ...... 12
3.6.4. Details of measures to be taken to minimise bias, such as randomisation, and management
of potential confounding factors. ..................................................................................................................... 13
3.6.5. Description of the clinical procedures and diagnostic methods relating to the clinical
investigation and in particular highlighting any deviation from normal clinical practice. ......................... 13
3.6.6. Monitoring plan ................................................................................................................................. 14
3.7. Statistical design and analysis ........................................................................................................ 15
3.8. Data management ............................................................................................................................ 16
3.9. Modifications of the CIP ................................................................................................................... 16
3.10. Deviations from the CIP ................................................................................................................... 17
3.11. Device accountability ....................................................................................................................... 17
3.12. Statements of compliance ............................................................................................................... 17
3.13. Informed consent process ............................................................................................................... 18
3.14. Adverse events, adverse device effects and device deficiencies ............................................. 18
3.15. End, suspension, or premature termination of the clinical investigation .................................. 19
3.16. Arrangements for subjects following participation ....................................................................... 20
3.17. Publication policy .............................................................................................................................. 20
3.18. Technical and functional features of the device ........................................................................... 20
3.19. Bibliography ....................................................................................................................................... 20

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
4
Abbreviations
ADE Adverse Device Effect
1
AE Adverse Event
2
CIP Clinical Investigation Plan
DD Device Deficiency
DMC Data Monitoring Committee
DSMB Data Safety Monitoring Board
EC Ethics Committee
EUDAMED European Database on Medical Devices
IB Investigator’s Brochure
IFU Instructions for use
ISO International Organization for Standardization
MDCG Medical Devices Coordination Group
MDR Medical Devices Regulation, (EU) regulation 2017/45 on medical devices
SADE Serious Adverse Device Effect
3
SAE Serious Adverse Event
4
SIN Single Identification Number
1
An adverse device effect is any adverse event related to the use of an investigational medical device or a
comparator if the comparator is a medical device.
2
Defined in article 2(57) of the MDR.
3
Any adverse device effect that has resulted in any of the consequences characteristic of a SAE.
4
Defined in article 2(58) of the MDR.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
5
1. Introduction
When a sponsor of a clinical investigation submits an application according to article 70(1) of the
MDR, to the Member State(s) in which the clinical investigation is to be conducted, the
application shall be accompanied by the documentation referred to in Chapter II of Annex XV of
the MDR.
According to section 2 of Chapter I of Annex XV of the MDR, clinical investigations shall be
performed on the basis of an appropriate plan of investigation reflecting the latest scientific and
technical knowledge, and defined in such a way to be able confirm or refute the manufacturer's
claims regarding the safety, performance and aspects relating to the benefit-risk determination
of devices. The clinical investigation shall include an adequate number of observations to
guarantee the scientific value and validity of the conclusions. The procedures and research
methodologies used to perform the clinical investigation shall be appropriate to the device under
investigation.
Section 3 of Chapter II of Annex XV of the MDR describes the legally required content of the
Clinical Investigation Plan (CIP). Further the sections 2.7 in chapter I, 3.12 chapter II as well as
4 and 6 in chapter III of Annex XV indicate that clinical investigations should be conducted in
accordance with good clinical practice.
The international standard ISO14155:2020 Clinical investigation of medical devices for human
subjects - Good clinical practice addresses good clinical practice for the design, conduct,
recording and reporting of clinical investigations. This standard has a normative Annex A that
outlines the content of a CIP. Adherence with the ISO 14155:2020 standard is strongly
recommended as it is a useful resource for sponsors when planning and developing their clinical
investigations, although it is not mandatory for clinical investigations conducted in accordance
with MDR. Note that standards are regularly updated, and it is foreseen that this guidance will
be updated accordingly.
When preparing the CIP, sponsors are encouraged to review the full details of the regulation as
well as the standard. In case there are discrepancies between MDR and the standard, the legal
requirements of the regulation takes precedence. The requirements of both the MDR and
ISO14155:2020 as well as experience from the competent authorities have been used to
develop this guidance document.
This guidance document is not legally binding. It has been developed following contribution from
national competent authorities, industry and relevant stakeholders and it should therefore be
recognised as best practice. It has been written to support sponsors developing their CIP by
describing in greater detail what type of information is expected in the respective CIP sections,
to pre-empt questions from the competent authorities during the assessment of the clinical
investigation application. Moreover, a CIP with the appropriate content will be instrumental in the
conduct of the clinical investigation.
The content of the CIP should be adapted based on the type of clinical investigation and the type
and development stage of the investigational medical device. The legal requirements in Section
3 of Chapter II of Annex XV of the MDR must be addressed or indicated as “not applicable” with
justification.
This guidance document uses section 3 of chapter II in Annex XV of the MDR as a starting point,
and follows the numbering of the regulation, in order to facilitate cross referencing to the legal
requirements. It is not intended to be a template for writing a CIP, and it is not mandatory to present
the information in a CIP in the same order as they are mentioned in the MDR or in this guidance.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
6
In combined studies of medical devices and pharmaceutical products, there is an obvious need
to accommodate the legal requirements from several regulations, and thus the structure and
content of the CIP may need to be adapted. However, sponsors need to be aware that the
elements required by MDR need to be present in a combined CIP/study protocol, and this
guidance is intended to be useful also in those situations.
2. Purpose of the CIP
The clinical investigation plan (CIP) shall set out the rationale, objectives, design methodology,
monitoring, conduct, record-keeping, and the method of analysis for the clinical investigation.
The CIP should be detailed enough to serve as a manual for investigators conducting the clinical
investigation in a consistent manner across investigational sites and over time. Further, the CIP
should allow the competent authorities and ethics committees to assess whether the clinical
investigation has been designed in such a way that potential risks to subjects or third persons,
after risk minimization, are justified when weighed against the clinical benefits to be expected.
The CIP should also allow the assessment of whether the reliability and robustness of the data
to be generated in the clinical investigation warrants the exposure of subjects to the
investigational device and procedures described in the CIP.
3. Content of the CIP
Note that it is preferred for all necessary information to be included in the CIP. If part of the
required information is provided in a separate document, it will be summarised and referenced
in the CIP. The referenced documents must be submitted together with the CIP as part of the
initial submission package accompanying the clinical investigation application.
3.1. General
The general introduction should include:
• The title of the clinical investigation.
• The CIP reference number(s)
5
.
• Version and date of the CIP.
• A summary of the revision history in case of modifications.
• Abbreviations and acronyms.
• An overall synopsis of the clinical investigation. For detailed guidance regarding content
of the synopsis, please refer to recommended template in Annex A of this guidance. Note
that information provided in the synopsis should also be detailed in the body of the CIP,
and that information which is mentioned more than once needs to be consistent
throughout the document. Further, it may be useful to include a graphic flow chart
describing the clinical investigation design.
Note the requirement in section 3.1, chapter II of Annex XV of the MDR to provide an overall
synopsis of the clinical investigation in an official Union language determined by the Member
5
The sponsor’s unique identifier such as CIP code/number, as well as the CIV-ID (issued by competent authority
from Eudamed2) or SIN (Single Identification Number – automatically generated when sponsors start to a draft
application in EUDAMED).

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
7
State concerned. Sponsors are advised to check national requirements in this regard and
provide one synopsis per language.
The name and contact details of the following should be stated:
• Sponsor.
• Legal representative (if applicable)
6
.
• Principal investigator(s).
• Coordinating investigator(s) (if applicable).
• Investigational sites in which the clinical investigation will be conducted.
• Other organisations such as central laboratories, clinical research organisations etc.
contracted by the sponsor as providers for the clinical investigation (if applicable).
• Manufacturer of investigational device.
The different roles, responsibilities and qualifications
7
of various kinds of investigators shall be
specified. In larger or more complex study setups, there may be several levels, e.g. co-ordinating
investigator, principal investigators, and members of the investigational site team. Further, in
case of combination studies, responsibilities and qualifications need to be clearly described for
the various investigators involved, e.g. investigators at clinical investigation sites where patients
are recruited and treated, vs investigators at the analysing sites for a performance study.
To facilitate updates, the names and contact details of the principal investigator(s) and
investigational sites can be listed in a separate document which is referenced in the CIP. Note
that in this case, it will be necessary to describe and maintain a procedure where an updated list
with names and contact details of sites is available to all investigators throughout the conduct of
the clinical investigation to facilitate communication, in, for example, emergency situations.
A brief description of the following must also be included:
• how the clinical investigation is financed.
• the agreement between the sponsor and the site(s).
A brief description of the agreement between the sponsor and the manufacturer of the
investigational device (if applicable) should be included.
The information about the agreements between parties may include for instance information
about providing investigational device(s) to the site as well as arrangements regarding
proprietary information and publications.
3.2. Identification and description of the investigational device
This section of the CIP should include the information listed below, as applicable. If appropriate,
references to the Investigator’s Brochure (IB) and/or Instructions for Use (IFU) can be made. In case
a comparator device is used the information below should also be provided for the comparator.
• Summary description of the investigational device including its intended purpose in the
clinical investigation as well as the populations and indications for which the
investigational device is intended.
6
The requirement for a sponsor to have a legal representative is described in article 62(2) of the MDR.
7
Refer to Article 62(6) of the MDR, Section 10.2 of ISO 14155:2020 and national provisions regarding investigator
qualifications.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
8
o If there is a known difference between the device’s intended
purpose/indication/population in the clinical investigation (due to development
stage, study design or other reasons) and the planned intended purpose when
the device is/will be placed on the market, this difference should be clearly stated.
o If the device has already been CE-marked and placed on the market, it should be
explained whether the intended purpose of the device in the clinical investigation
is different from the intended purpose for which the device has been CE marked,
or if it is to be further assessed within the scope of its intended purpose. This
should be clearly specified.
• Sponsors are recommended to also include the information required by Section 3.18,
chapter II Annex XV of the MDR in the device description, i.e. to list the technical and
functional features of the device, with specific mention of those covered by the
investigation. Please refer to section 3.18 of this document for further guidance.
• Details concerning the manufacturer of the investigational device.
• Name or number of the model/type, including software version and accessories, if any,
to permit full identification.
• Description as to how traceability will be achieved during and after the clinical investigation,
for example, by assignment of lot numbers, batch numbers or serial numbers.
• A detailed description of the investigational device, including a list of all materials which
will be in contact with tissues or body fluids. Also, any medicinal substances, human or
animal tissues or their derivates, or other biological active substances incorporated in the
device must be defined.
• Summary of the necessary training and experience needed to use the investigational
device based on risk assessment.
• Description of the specific medical or surgical procedures involved in the use of the
investigational device.
• A background literature review should be presented.
3.3. Benefits and risks of the investigational device, clinical
procedures and clinical investigation
3.3.1. Benefits
A description should be provided of the potential benefits of the proposed clinical investigation.
This concerns the direct benefit(s) to the study subjects but may also cover the benefit(s) to others.
In particular, regarding the direct and indirect benefit(s) to the study subject, the following factors
should be considered, individually and in aggregate:
a) type of benefit(s) and estimated magnitude of the benefit(s).
b) if possible, probability evaluation of the subject experiencing one or more benefits, or
identification of subgroups more likely to experience a benefit.
c) duration of the benefit(s), i.e., how long the benefit can be expected to last for the subject.
d) medical necessity, if a medical device provides benefits or addresses needs unmet by
other medical devices or therapies.
Benefit considerations should also include an assessment of whether another medical device or
therapy could be used in substitution, and the availability of that other medical device or therapy.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
9
It may be necessary to take regional differences in availability of alternatives into account, which
could lead to benefit considerations that vary by region.
Benefit(s) to others include(s) benefits to caregivers, family members, health care personnel,
and public health.
Other information providing useful context is appreciated and may include consideration of
patient preference information (when available) characterizing the subjects’ perspective on
benefit, i.e., the value that the patients place on the use of the medical device, as well as
information characterizing subjects’ tolerance for risk.
Please note that there are specific requirements for vulnerable populations and subjects that
there should be scientific grounds for expecting that participation in the clinical investigation will
produce a direct benefit (see article 64-66 and 68 of the MDR).
3.3.2. Risks
Identify all risks which participation in the clinical investigation will result in subjects being
exposed to, whether related to the investigational device or clinical investigation procedures (i.e.,
risk characterization). Possible interactions with concomitant medical treatments have to be
considered.
In particular, for risk characterization, the following should be considered, individually and in
aggregate: types of risk (taking account of the study design as well), their likelihood (probability
of occurrence) and duration along with the severity of harm.
Also consider the risk factors for health care personnel, family members or caregivers, if any.
Also, consider the risks related to the interpretation of the study data. Specifically, the risk of
drawing a false conclusion based on clinical data obtained, and the risks associated with data
which are inconclusive or difficult to interpret should be considered.
Also describe how the risks are minimised (i.e., risk mitigation). It is not necessary to include
specific mitigations for risks that are determined to be negligible due to a low probability of
occurrence and low severity of harm. However, it is expected that all possible risks are identified.
Non-negligible identified risks should be reduced as far as possible by the following measures,
and in the following priority:
• Risk elimination/reduction through safe design and manufacture of the device. This
involves identifying device risks through pre-clinical testing and making changes in
design or manufacturing in advance of the clinical investigation. Verification and
validation of device design should be conducted prior to commencement of the clinical
investigation application.
• Protective measures such as physical protective measures or alarms.
• Communication of safety information, contraindications and residual risks (e.g., through
labelling or informed consent), training of health care professionals/investigational staff,
optimizing communication between sponsor and the participating sites as well as
sponsor optimizing the transfer of relevant information between the sites, communicating
safety data and residual risks with ethics committee(s) and competent authority to
determine if any additional subject protection measures are needed.
Any residual risks related to the device, or the investigation should be mitigated by safe clinical
investigation design. Any non-negligible risks which remain following device design and are
mitigated by protective measures or communication of safety information should be considered

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
10
in the clinical investigation design and mitigated further if possible. Examples of how clinical
investigation design can contribute to risk mitigation:
• Designing the clinical investigation to be conducted in accordance with relevant
international standards, consensus guidance, and good clinical practice.
• Performance of the study at specialised clinical sites only, with investigators meeting
specific specialist criteria.
• Staged enrolment and interim pre-specified subject safety assessment.
• The use of pre-specified stopping rules.
• Enrolling a narrow study population with more favourable benefit-risk profile.
• Study oversight involving expert independent monitoring committees.
• Frequent monitoring visits to the site(s) ensuring accurate recording of AEs, including the
timing and clinical context and a description of any medical interventions provided and
the associated outcomes, as well as compliance with safety reporting requirements.
The risks listed should align, to a relevant extent, with the list of anticipated A(D)E, SA(D)E, DD
with SADE potential as mentioned in section 3.14.
For CE-marked devices (including comparators) a brief summary of the post market surveillance
data available is of relevance.
The CIP should describe how the risk threshold and the degree of distress is defined and
constantly monitored throughout the investigation, as required by the MDR
8
.
3.3.3. Benefit-risk ratio
Summarize the rationale for the benefit-risk ratio of the clinical investigation, taking into account
the conditions stated in articles 62(3) and 62(4)e of the MDR. Overall, the investigation must be
designed to involve as little pain, discomfort, fear and any other foreseeable risk as possible for
the subjects. For that, a rationale in relation to the available preclinical data and results of clinical
evaluation is recommended.
For clinical investigations carried out with vulnerable populations (incapacitated persons, minor,
pregnant or breastfeeding women) clearly explain if the clinical investigation involves an
expected direct benefit for the subject
9
). In case of a clinical investigation in an emergency
situation
10
, it should be explained if the clinical investigation will have the potential to produce a
direct clinically relevant benefit to the subject. In addition, it must be justified that the clinical
investigation poses a minimal risk to, and imposes a minimal burden on, the subject in
comparison with the standard treatment of the patient's condition.
3.4. Relevance of the clinical investigation
Describe the relevance of the clinical investigation in the context of the state of the art of clinical
practice.
8
Article 62(4)i of the MDR.
9
Articles 64-66 of the MDR.
10
Article 68 of the MDR.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
11
The justification for the design of the clinical investigation should be based on the conclusions
of the clinical evaluation
11
. Summarize the evaluation of the relevant pre-clinical
testing/assessment and any prior clinical investigations, to justify the use of the investigational
device in human subjects. (if applicable). Provide an evaluation of clinical data that are relevant
to the proposed clinical investigation.
Describe where the clinical investigation fits into the clinical development of the device (i.e., is
this a pilot study, a pivotal study or a post-market clinical investigation?). The informative Annex
I in ISO 14155:2020 has information on clinical development stages.
3.5. Objectives and hypotheses
The purpose of the clinical investigation, claims for clinical performance, effectiveness or safety
of the investigational device that are to be verified should be described.
• Objectives are to be identified as primary, secondary and exploratory as relevant. If
applicable, describe whether ‘superiority’, ‘non-inferiority’, or ‘equivalence’ is to be
demonstrated.
• Include scientific justification and clinical relevance for effect sizes, non-inferiority
margins or equivalence limits, where applicable.
• Primary and secondary hypothesis, if applicable.
• Risks and anticipated adverse device effects that are to be assessed.
The objective(s) shall serve the purpose of the clinical investigation and shall relate to the
hypotheses (where applicable) and to the corresponding endpoints that shall be relevant to the
target population.
The endpoints of the clinical investigation shall address the intended purpose, clinical benefits,
performance and safety of the device. The endpoints shall be determined and assessed using
scientifically valid methodologies. The primary endpoint shall be appropriate to the device,
clinically relevant and should be evaluable.
3.6. Design of the clinical investigation
The design should be sufficiently detailed with evidence of its scientific robustness and validity.
3.6.1. General information such as type of investigation with rationale for
choosing it, for its endpoints and for its variables as set out in the
clinical evaluation plan
• Indicate the study type (e.g., exploratory, confirmatory).
• Define the primary and secondary endpoints, with rationale for their selection and
measurement, highlighting the endpoints that address safety and/or performance, as well
as clinical benefit(s) of the device. If applicable, composite endpoints
12
, with rationale for
their selection and measurement should be justified.
• For certain investigations, in particular early studies of new/high risk devices additional
safety measures should be considered, such as close monitoring by the sponsor and
11
For details on clinical evaluation, refer to article 61 and Annex XIV of the MDR. The sponsor should also consult
relevant MDCG guidance documents and section 6.3 of ISO 14155:2020.
12
Composite endpoint is a pre-specified combination of more than one endpoint.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
12
independent safety monitor, and limiting the rate of enrolment (e.g.; the study design
could include an evaluation of the first patient before next patient is treated, a phased
approach, use of a run-in component).
• Indicate the expected duration of the investigation, for each subject’s participation and
the estimated total duration of the clinical investigation.
3.6.2. Information on the investigational device and any comparator to be
used in the clinical investigation.
• Present the study arms, i.e. the investigational device (which was presented in detail as
outlined above in section 3.2) versus any comparator (other device, medication,
treatment modality or sham procedure) used. The choice of, or absence of, comparator,
should be justified.
• In case of implantable devices, the sponsor should provide subjects with an implant card.
The content of the card and a description of when and how it is provided should be
addressed in the CIP, considering relevant aspects of article 18 of the MDR.
3.6.3. Information on subjects, selection criteria, size of investigation
population, representativeness of investigation population in relation to
target population and, if applicable, information on vulnerable subjects
involved such as children, pregnant women, immuno-compromised or
elderly subjects.
• Indicate the number of subjects: The planned total number of subjects, as well as the
distribution between study arms if applicable.
• Specify if the clinical investigation will include vulnerable subjects
13
such as children,
pregnant and breast-feeding women, incapacitated, immunocompromised or elderly
subjects or other subjects which may be deemed vulnerable.
• List the subject selection criteria, (i.e. specify inclusion and exclusion criteria), and
indicate who is responsible for determining subject eligibility (i.e. define role and
qualification).
• Describe the recruitment procedures, including when a subject is enrolled and if
applicable, specify the time point of subject randomisation (which may be different from
the time of enrolment) in the clinical investigation.
• Note the requirement
14
to perform clinical investigations in a clinical environment that is
representative of the normal conditions of use of the device in the target patient
population.
o Discuss the representativeness of the investigation population in relation to the
intended target population. The design may include consideration of, and
justification for, aspects such as disease aetiology, disease severity, gender, age
(e.g. adult, paediatric) and other special patient populations as appropriate.
o Discuss the type of investigation sites (e.g. specialized clinic, primary health care
centre, manufacturer’s custom built facility etc.) and differences in investigation
site environments. Elaborate on why the selected sites are deemed appropriate
for the conduct of the clinical investigation.
o In multicentre/multinational studies it might be necessary to consider any
expected differences in the standard of care or patient outcomes based upon the
13
Article 62(4)(d), articles 64-68 as well as section 3.6.3 in chapter II, Annex XV of the MDR relate to vulnerable
subjects.
14
Section 2.4 in chapter I, Annex XV of the MDR.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
13
geographic distribution of the intended patient or user populations. Discuss the
impact and account for any local adaptations.
• Describe whether patients were or will be involved during the different phases of the
clinical investigation, e.g. involvement in determining the objectives, assessing the
burden of study participation for subjects or dissemination of the results.
3.6.4. Details of measures to be taken to minimise bias, such as
randomisation, and management of potential confounding factors.
• Describe measures taken to minimize bias or avoid bias, such as randomization,
concealment of allocation, blinding/masking, and management of potential confounding
factors. Use of either single arm or (choice of) comparator or other (historically) controlled
design and the concept of blinding and unblinding, or running open label need to be
covered, with rationale and justification.
• Sham procedures (if any) need to be thoroughly justified, in particular if the procedures
are invasive or burdensome, as exposing subjects to risk without the potential benefit of
the device/intervention may be questionable from an ethical perspective.
• Be transparent about any potential conflicts of interest, and if they are present, how these
shall be managed. In particular, it needs to be discussed how undue influence on
subjects and evaluation of endpoints can be avoided, for example in situations where the
device inventors are closely involved in the conduct of the investigation. To avoid bias in
certain assessments an independent committee may be used to determine eligibility,
classification of events, endpoint adjudication etc. (clinical events committee (CEC)).
• Further a data safety monitoring board (DSMB) or data monitoring committee (DMC)
should be considered, and in appropriate situations, appointed to continuously monitor
the emerging clinical investigation results and advice on the termination or progression
of the study.
• If the clinical investigation involves a blinding/ masking technique, include criteria for who
will get access to and is authorised to break the blinding/masking code, and the
circumstances when this would occur.
3.6.5. Description of the clinical procedures and diagnostic methods relating
to the clinical investigation and in particular highlighting any deviation
from normal clinical practice.
• Describe all the clinical investigation -related procedures and diagnostic methods used
in the clinical investigation. Any deviation from normal clinical practice should be
highlighted. A tabular overview/schedule of events may be helpful to summarise the
activities by visit, but it also needs to be clearly presented in detail what will have to be
performed at which visit, in which order, how and by whom.
• The number of medical devices and comparators (if applicable) used per subject, and
procedures to ensure safe use of the device need to be described, in particular in
situations where the same device is used for several subjects.
• Methods and timing for assessing, recording, and analysing variables (such as adverse
events, symptoms, parameters and/or results to be studied), including details on the
equipment to be used for assessing the clinical investigation variables and arrangements
for monitoring the maintenance and calibration of such equipment.
• Specify which biological samples are collected for the purpose of the clinical
investigation, if any, and describe the arrangements to comply with the applicable rules
for the collection, storage and future use of biological samples.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
14
• Follow-up of subjects: The follow-up period during the clinical investigation shall permit
the demonstration of clinical performance, effectiveness, or safety over a period of time
sufficient to represent a realistic test of the investigational device and allow any risks
associated with adverse device effects to be identified and assessed.
• Any concomitant treatments permitted or prohibited should be explicitly stated
(remember to consider contraindications and interactions not only for the investigational
device but also for comparators and required concomitant treatments).
• If applicable, lifestyle restrictions such as contraception measures or diet restrictions
should be described.
• Criteria and procedures for subject withdrawal or lost to follow-up: Describe when and
how to withdraw a subject from the clinical investigation or stop the use of the
investigational device, efforts to be made to trace subjects that are lost to follow-up and
possible reasons, as well as information on whether and how subjects are to be replaced.
It is recommended to consider the need for a last safety follow-up visit (if relevant for the
clinical investigation and accepted by the subject) for subjects that withdraw from use of
the device and/or other follow up activities defined in the CIP.
• Address whether the subjects can continue the use of the medical device once the clinical
investigation has been completed, if applicable.
• Clinical investigations of implantable devices need to address procedures for
explantation (including return and analysis of explants obtained at explantation or post-
mortem examinations) and in situations where implants are left in situ, the monitoring of
patient safety beyond the study period needs to be ensured.
3.6.6. Monitoring plan
The sponsor shall ensure adequate monitoring of the clinical investigation to verify that the rights,
safety and well-being of subjects are protected, that the reported data are reliable, and robust,
and that the conduct of the clinical investigation is in compliance with the requirements of MDR
15
and standard for good clinical practice (GCP).
The CIP shall contain information on the monitoring plan.
16
It is acknowledged that a detailed
monitoring plan may not have to be provided with the application. The monitoring plan can be a
separate document, as determined by the sponsor, but the CIP should include at least the
following:
• A general outline of the monitoring plan.
• A description of the appointment of a monitor that is independent from the investigational
site.
• A description of the monitor’s access to source data and the extent of source data
verification planned.
The extent and nature of monitoring the conduct of the investigation in accordance with the
clinical investigation plan, good clinical practice and the MDR should be based on the
characteristics of the clinical investigation, including objective(s) and methodology of the clinical
investigation and degree of deviation of the intervention from normal clinical practice.
15
Article 72(2) of the MDR.
16
Section 3.6.6, chapter II, Annex XV of the MDR.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
15
3.7. Statistical design and analysis
The CIP shall describe and justify the statistical design and analysis of the clinical investigation
and should cover following points, if applicable:
• Analysis population and procedures that take into account all the data.
• Descriptive statistics of baseline data, treatments, safety data and where applicable,
primary and secondary endpoints.
• Analytical procedures including measures of precision such as confidence intervals.
• With regards to the primary endpoint, the statistical testing strategy should be presented,
if applicable, including the power calculation and the level at which statistical significance
will be claimed.
• Sample size calculation and justification considering:
o all relevant clinical data on the outcome variable and effect size, if applicable;
o assumptions about expected outcomes in the treatment groups, where applicable;
o adjustments due to pre-planned interim analyses, if any;
o the magnitude of the detectable effects and the non-inferiority margin, which must be
smaller than the magnitude of the detectable effects and be justified in relation to the
comparator effect, if applicable;
o the allocation ratio used for randomisation (e.g. 1:1, 1:2) if applicable;
o the expected drop-out rate, such as withdrawal, loss of sight, death (unless death is
an endpoint).
All statistical parameters and methods used to calculate the sample size or non-inferiority
margin should be clearly stated.
For exploratory and observational clinical investigations, where sample size
determination by calculation is not required per Annex I of the ISO14155:2020 standard,
the scientific justification for the sample size selected should be provided.
• The rationale for the number of procedures to be performed by a single user as part of
the learning curve and how these data are to be analysed, if applicable.
• Pass/fail criteria to be applied to the results of the clinical investigation.
• The provision for interim analyses, if applicable, and the provision of objective,
quantifiable, statistical criteria for the termination of the clinical investigation
17
.
• Management of bias and, when randomization, matching, or blinding are applied, plan of
assessment of success thereof. Strategies to manage and control for potential
confounding factors (e.g. stratified randomisation or stratification of the analysis). These
strategies should be justified.
• For multicentre clinical investigations, a strategy for handling the potential imbalance of
the numbers of subjects across investigation sites.
• Description of procedures for multiplicity control and adjustment of error probabilities.
• The specification and justification of subgroups for analysis, including specification of
whether response to treatment is expected to be different in these groups.
• Management, justification, and documentation of missing, unused or spurious data,
including drop-outs.
• Exploratory analysis and sensitivity analysis (e.g. to explore robustness of results of
primary and secondary analysis with respect to different methods used for handling
missing data).
• Procedures for reporting any deviations(s) from the original statistical plan.
• A strategy for pooling data, if applicable.
17
There could also be non-statistical grounds for termination of a clinical investigation.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
16
It is recommended to consult appropriate statistical expertise when designing the clinical
investigation and writing the clinical investigation plan.
3.8. Data management
In the clinical investigation plan, a description should be provided of the procedures implemented
which can guarantee that the data generated in the clinical investigation is reliable and robust.
Present the arrangements to record, process, handle and store data in such a way that it can be
accurately reported, interpreted and verified while the confidentiality of records and the personal
data of the subjects remain protected in accordance with the applicable law on personal data
protection. Present post-collection procedures to check data accuracy and completeness, as
well as procedures for issuing and resolving data queries and methods for data base locking at
the start of the analysis.
18
Throughout, and after the completion of, the clinical investigation, appropriate technical and
organizational measures should be installed to protect information and personal data processed
against unauthorized or unlawful access, disclosure, dissemination, alteration, or destruction or
accidental loss, in particular where the processing involves transmission over a network.
The MDR specifically requires
19
that the application for a clinical investigation includes a
description of measures that will be implemented in case of a data security breach in order to
mitigate the possible adverse effects. The data management section of the CIP is a reasonable
place to include this information, or a separate document can be included.
Also the data retention requirements as specified in section 3 of chapter III in Annex XV of the
MDR should be addressed.
3.9. Modifications of the CIP
It should be clear from the clinical investigation plan that, the competent authority
20
shall be
notified of all proposed changes to the approved clinical investigation that are likely to have a
substantial impact on the safety, health or rights of the subjects or on the robustness or reliability
of the clinical data generated by the investigation, as required in Article 75 of the MDR. Also the
CIP should inform the investigator of the need to wait for the time specified in article 75 of the
MDR or for the approval of the substantial modification, whichever comes first, before
implementing the changes.
The procedures to manage non-substantial modifications to the CIP also needs to be described.
18
Refer to sections 6.6, 7.8 and A.8 of the ISO14155:2020 for additional guidance on data management aspects.
19
last indent of section 4.5, chapter II in Annex XV of the MDR.
20
Note that it may be necessary to take into consideration also national requirements in relation to submission of
substantial modifications to the Ethics Committee.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
17
3.10. Deviations from the CIP
There should be a statement specifying that the investigator is not allowed to deviate from the
CIP, except if to protect the rights, safety and well-being of human subjects under emergency
circumstances, when the investigator may deviate without prior approval of the sponsor.
It further needs to be clearly stated in the CIP that waivers from the CIP are not permitted.
Procedures for recording, reporting, and analysing CIP deviations should be described, including
notification requirements and time frames. Also, corrective and preventive actions and principal
investigator disqualification criteria are to be included.
3.11. Device accountability
Adequate procedures for the accountability and traceability of the investigational device should
be incorporated in the CIP, in particular control of access to and adequate storage of the device,
follow-up in relation to the device used in the clinical investigation and the return of unused,
expired or malfunctioning devices.
Describe in detail how the use of the investigational device is restricted, so that they are used
only in the clinical investigation and according to the CIP
21
. Specify that the investigator shall
keep records to document
• name(s) of person(s) who received, used, returned, or disposed of the device.
• the date of receipt, identification, and quantity of each investigational device (batch
number/serial number or unique code).
• the expiry date, if applicable; d) the date or dates of use.
• subject identification;.
• date on which the investigational device was returned/explanted from subject, if
applicable.
• the date of return of unused, expired, or malfunctioning investigational devices, if
applicable.
• the date and documentation of disposal of the investigational devices as per instructions
of the sponsor, if applicable.
3.12. Statements of compliance
The following statements should be included in the CIP:
• Statement specifying that the clinical investigation shall be conducted in accordance with
the ethical principles that have their origin in the Declaration of Helsinki.
• Statement specifying compliance with any relevant international standards and/or
consensus guidance, such as the latest version of the international standard ISO 14155
Clinical investigation of medical devices for human subjects – Good clinical practice
22
• Statement specifying compliance with the national legislation and MDR.
21
It may be acceptable to make exemptions regarding device accountability for those clinical investigations where
CE marked devices are used within their intended purpose.
22
If the sponsor chooses not to comply with this standard, it is necessary to demonstrate that the alternative
solutions do ensure sufficient protection of the rights, safety and well-being of subjects, the scientific conduct of
the clinical investigation and the credibility of the clinical investigation results at a level that is equal or superior to
the methods specified in the standard.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
18
• Statement specifying that the clinical investigation shall not begin until the required
regulatory and ethical assessments have been completed with non-negative outcomes,
in accordance with MDR and national legislation.
• Statement specifying that any additional requirements imposed by the Ethics Committee
or regulatory authority shall be followed, if appropriate.
• Statement specifying the type of insurance that shall be provided for subjects, if
appropriate.
3.13. Informed consent process
Describe the general process for obtaining informed consent, including the process for providing
subjects with new information and process for compensation to subjects for participation in the
clinical investigation, as needed. If applicable, the description of the process in circumstances
where the subject is unable to give informed consent must also be included.
For clinical investigations on minors, the CIP must provide a summary of how it meets MDR
Article (65) requirements, including the informed consent of the minor’s legally designated
representative, and the provision of information to the minor in a way that is adapted to their age
and mental maturity.
For clinical investigations in emergency situations, it should be justified why and how the
conditions in article 68 of the MDR, that allow inclusion of subjects and a first intervention without
a prior informed consent, are considered to be fulfilled. Describe the planned procedures to
identify a legally designated representative for such subjects to ensure that informed consent
can be obtained without undue delay either from the legally designated representative or the
subject, whichever can be done sooner. National legislation in appointing legally designated
representatives differs. To ensure compliance with national provisions it is necessary for the
sponsor to provide the investigators with appropriate guidance on how to proceed in their
country. For multinational investigations, the information could be provided as a country specific
appendix to the CIP.
3.14. Adverse events, adverse device effects and device deficiencies
List the definitions of adverse events (AE), adverse device effects (ADE), device deficiencies
(DD), serious adverse events (SAE) and serious adverse device effects (SADE). Note the
requirements for recording and reporting of adverse events in article 80 of the MDR, and consult
the guidance document MDCG 2020-10/1
23
for definitions and more information on the reporting
of SAE and DD.
A list of foreseeable adverse events and anticipated adverse device effects, together with their
likely probability of occurrence, mitigation, or treatment must be specified.
Should the sponsor wish to exclude some adverse events from recording and/or reporting, these
should be listed, and a rationale provided for why they are to be considered non-reportable.
Details of the process for recording, follow-up and reporting adverse events and device
deficiencies should be described, including the time frame which the principal investigator must
report to the sponsor and, where appropriate, the sponsor must report to the competent
23
MDCG 2020-10/1 Rev 1 Safety reporting in clinical investigations of medical devices under the Regulation (EU)
2017/745

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
19
authority. Emergency contact details for reporting SAE and SADE must be specified, so that the
investigator knows whom to contact.
Information on the presence or absence of a data safety monitoring board/data monitoring
committee
24
(DSMB/DMC) should be provided. In case of the absence of a DSMB/DMC, a
justification should be provided.
3.15. End, suspension, or premature termination of the clinical
investigation
Define the end of the clinical investigation. The end of investigation definition is important in
relation to reporting requirements at the end of the study as outlined in article 77 of the MDR.
The clinical investigation plan should consider appropriate stopping criteria on both subject and
study level. Consider that depending on the situation, it might be necessary to stop recruitment
of new subjects and treatment of subjects currently exposed to the device, but also necessary
to continue follow up of already treated/ implanted patients. Procedures should be described for
the follow-up and continuing care of subjects following the end or temporary halt of the
investigation. If applicable, procedures should be described for follow-up of subjects who have
withdrawn their consent and for subjects lost to follow-up. For implantable devices it should be
specified whether the devices are to remain implanted or be explanted at the end of the study
and how traceability is achieved.
Include a description of any required follow-up (incl. the duration of such a follow-up period) of
SAE with a causal relationship with the investigational device, still ongoing at the end of the
clinical investigation, based on a risk assessment by the sponsor of the characteristics and
properties of the investigation and the investigational device. This description should also include
how any potential new SAEs that are detected during such follow-up are to be handled.
Further, it must be clear from the clinical investigation plan that the competent authority shall be
notified of the temporary halt or (premature) end of the clinical investigation, and that a
justification shall be provided in case of a temporary study halt or early termination. In
accordance with MDR article 77 study (premature) end or temporary halt reporting is mandatory
within 15 days (or 24 hours if based on safety grounds).
In addition, a clinical investigation report needs to be submitted to the competent authority
25
within one year of the end of the clinical investigation or within three months of the early
termination or temporary halt. The clinical investigation report shall be accompanied by a
summary presented in terms that are easily understandable to the intended user. Refer to the
Commission Guidance on the content and structure of the clinical investigation report (2023/C
163/06).
24
A data monitoring committee can be established by the sponsor to assess at intervals, the progress of the clinical
investigation, the safety data or the critical clinical performance or effectiveness endpoints and to recommend the
sponsor whether to continue, suspend, modify, or stop the clinical investigation. Sponsor can pre-empt requests
for information from the competent authorities during the assessment of the clinical investigation application by
submitting the DSMB charter with the initial application.
25
Note that it may be necessary to consider also national requirements regarding reporting at the end of the clinical
investigation which may include reporting to the Ethics Committee.

Medical Device
Medical Device Coordination Group Document MDCG 2024-3
20
3.16. Arrangements for subjects following participation
Describe the arrangements for taking care of the subjects after their participation in the clinical
investigation has ended, where such additional care is necessary because of the subjects’
participation in the clinical investigation and where it differs from that normally expected for the
medical condition in question.
3.17. Publication policy
Following statements must be included:
• Statement that the clinical investigation will be registered in a publicly available
database
26
.
• Statement indicating that the results of the clinical investigation will be made publicly
available.
• Statement indicating the conditions and timeframes under which the results of the clinical
investigation will be offered for publication including the role of the sponsor and criteria
for authorship.
3.18. Technical and functional features of the device
List the technical and functional features of the device and specify those features which are
studied in the clinical investigation.
A tabular presentation of the relevant product characteristics of the investigational device is
expected with an indication of the associated product specifications and assignment of the
expected clinical outcome. Please, state the expected clinical performance outcomes
specifically (e.g., according to the clinical investigation endpoints) and generally (whether it is a
safety or performance characteristic).
Depending on the level of complexity, this information could be integrated with other sections,
such as the device description and/or endpoint (refer to sections 3.2 and 3.6.1 above) or may
need to be presented in a separate section.
3.19. Bibliography
List of bibliographic references relating to the clinical investigation.
26
Once EUDAMED is fully functional, the clinical investigations will be registered there upon application, but until
EUDAMED is fully functional, sponsors will have to register the clinical investigation elsewhere to be compliant with
article 35 of the Declaration of Helsinki and section 5.4 of ISO14155:2020.
Medical Device
Medical Device Coordination Group Document MDCG 2024-3
21
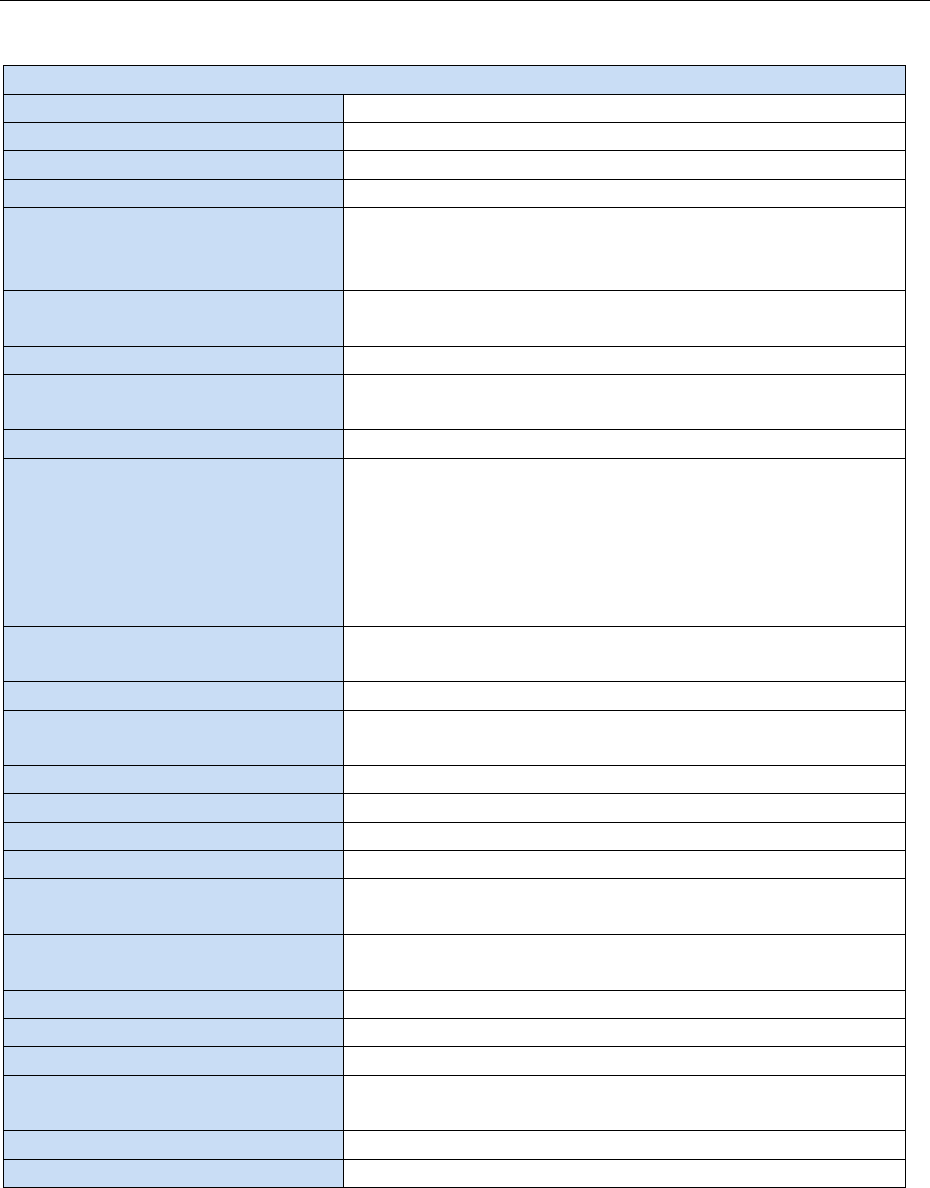
Appendix A: Clinical Investigation Plan Synopsis Template
Clinical Investigation Synopsis (Template)
Title
[enter text here]
Short title
[enter text here]
Lay title, if applicable
[enter text here]
CIP number, version, and date
[enter text here]
EUDAMED Single Reference
Number (SRN) or CIV-ID, if
previously assigned
[enter text here]
CI modification number, if
applicable
[enter text here]
Sponsor name and address
[enter text here]
Participating Location(s) and
country(ies)
[enter text here]
Name of Investigational Device
[enter text here]
Clinical investigation Purpose
and Background
• Rationale for CI
• Background of device and
condition
• Current standard of care
[enter text here]
Name of Comparator, if
applicable
[enter text here]
Clinical development stage
[enter text here]
Design of the clinical
investigation
[enter text here]
Objectives
[enter text here]
Primary endpoints
[enter text here]
Secondary endpoints
[enter text here]
Safety endpoints
[enter text here]
Exploratory / Other endpoints
and outcomes
[enter text here]
Description of participants /
study population
[enter text here]
Inclusion criteria
[enter text here]
Exclusion criteria
[enter text here]
Sample size
[enter text here]
Duration and follow up of the
clinical investigation
[enter text here]
Statistical considerations
[enter text here]
Note: For combination studies, more details may be relevant, such as EU number of the clinical
trial, name and description of investigational medicinal product or CIV-ID/SRN of performance
study of an in vitro diagnostic device.
